Work package 4
WP4: Clinical profile
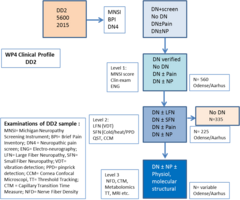
Clinical Profile. This work plan will determine the presence of pain and sensory abnormalities in the ADDITION and DD2 cohorts and a cohort of patients from Oxford, UK, using multiple techniques to achieve a singular goal: increasing our understanding of the pathophysiology of pain in type 1 and type 2 diabetic neuropathy. Ten percent of patients from the DD2 cohort sample will be invited for examination to participate in studies described in WP4.1-4 (see figure). We will also identify a comparable cohort of type 1 diabetes patients for examination.
WP4.1
In diabetes patients with painful and non-painful neuropathy from Oxford and Denmark, we will use the MNSI, standardised quantitative sensory testing (QST), neurophysiological assessments, and skin biopsies to determine the structural and functional differences between type 2 diabetes patients with and without pain.
WP4.2
To examine the role of autonomic function for pain in diabetic neuropathy, we will follow patients from the ADDITION study examined 6 years after the start of the project where 777 patients were tested for cardiac autonomic neuropathy. These tests will be repeated in 2015 to determine the progression of autonomic function and potential association to painful diabetic neuropathy. A more detailed assessment of autonomic functions will be done in a subsample using a series of techniques.
WP4.3
Using the well-phenotyped Oxford and Danish Cohorts, sensory function from deep somatic structures will be measured using pressure algometry. We will develop techniques to quantify small nerve fibres from muscle biopsies similar to that done for skin biopsies and correlate this to deep pain sensitivity in patients.
WP4.4
Case series of type 1 diabetic neuropathy patients from the three clinical sites (Oxford, Odense, and Denmark) will be compared with a sex- and age-matched type 2 diabetic neuropathy group to determine possible differences in structural and functional profile between type 1 and type 2 diabetic neuropathy. Also, these groups of patients will be asked to participate in studies for capillary nerve blood flow examination as well as metabolic analysis.
Threshold tracking provides information on the activity of ion channels and ion exchange processes and will be used to study axonal excitability, which is important for both motor and sensory nerve function in diabetic neuropathy. These studies will be done on well-phenotyped Oxford and Danish Cohorts.